Baby Born Womb Transplant: 'Miracle' Hugo Marks First UK Birth from Deceased Donor
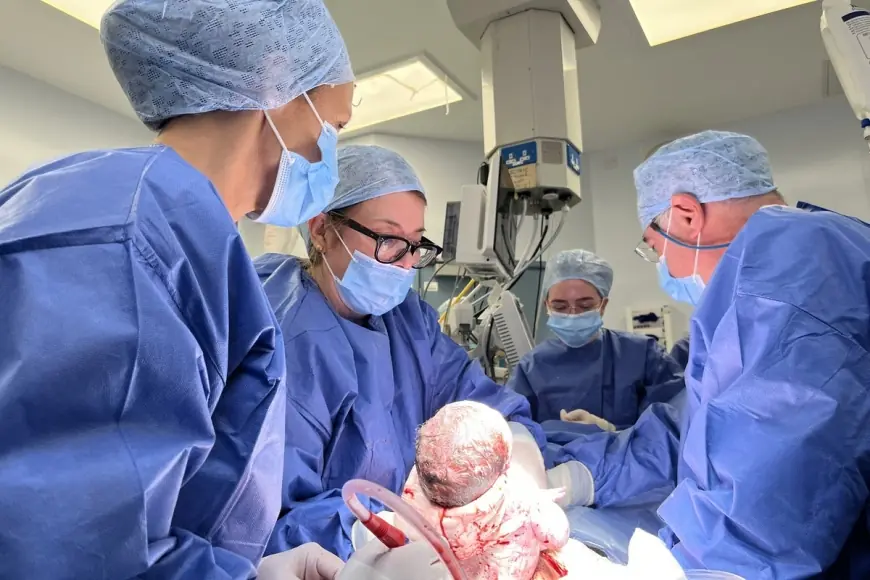
Grace Bell, in her 30s, has given birth to Hugo after receiving a womb transplanted from a deceased donor — a Baby Born Womb Transplant that marks the first such birth in the UK and a milestone in a clinical research trial.
Baby Born Womb Transplant — the birth and immediate reaction
Hugo was delivered just before Christmas 2025 at Queen Charlotte's and Chelsea Hospital in west London, weighing nearly 7lbs and specifically recorded at 6lb 13oz (3. 1kg). Grace Bell, who was born without a viable womb, called the arrival of her son simply a miracle and described waking after the birth and seeing his small face as dreamlike. Bell and her partner Steve Powell, from Kent, paid tribute to the donor and the donor family for what they described as an incredible gift; the partner is also referred to elsewhere as Steven Powell.
The transplant and IVF pathway
Bell's womb transplant operation lasted 10 hours and took place at The Churchill Hospital in Oxford in June 2024. Some months after the transplant she underwent IVF treatment and an embryo transfer at The Lister Fertility Clinic in London, leading to the successful pregnancy and delivery of Hugo.
Clinical team, timing and technical hurdles
More than 30 expert staff are involved in the care of each womb transplant patient, with clinicians describing the birth as a ground-breaking moment that could give hope to many women with similar diagnoses. Isabel Quiroga, consultant surgeon and clinical lead for organ retrieval at the Oxford Transplant Centre, part of Oxford University Hospitals, has carried out both womb transplants in the UK and highlighted that there is a precious amount of time during which a womb from a deceased donor can be used — the team estimates that time period to be about 12 hours.
Quiroga noted that, internationally, early failures after transplants from deceased donors are more common than after transplants from living donors, and that relatively few babies to date have been born after deceased donor womb transplants. Nonetheless, the success with Hugo — described as the third such birth in Europe and the first in the UK — demonstrates the possibility of expanding access to mothers who do not have living donors.
Patient experience and monitoring
Women who undergo womb transplants must attend additional appointments, receive extra scans to monitor fetal growth inside the transplanted womb, and have regular blood tests throughout the process. Clinicians involved in these cases emphasise that while worldwide experience is limited, many clinical skills used in caring for other organ transplant patients transfer to the management of complex pregnancies after womb transplantation.
Bryony Jones, a consultant obstetrician at Imperial College Healthcare NHS Trust who has delivered both babies born in the UK following womb transplants, said the whole team was present and delighted on the day of delivery. Teams providing care give time voluntarily through the charity Womb Transplant UK and are open with patients about the experimental and research aspects of the programme.
Donor families, trial status and wider implications
Bell has said she thinks of the donor and the donor's family every day and hopes they find peace in knowing their daughter enabled her to become a mother. Clinicians expressed deep gratitude to donor families, describing their generosity as allowing life and health to be given to others.
Bell's successful transplant is one of 10 such procedures carried out as part of a UK clinical research trial; three transplants have already been carried out under the trial, and this is the first birth arising from the programme. The team and investigators view the outcome as important for women who lack living donors and as an encouragement to continue carefully monitored research in this area.
What this means next
The medical teams involved characterise the event as a ground-breaking moment while noting ongoing uncertainties and the experimental nature of womb transplantation from deceased donors. Further monitoring of patients in the trial and continued evaluation of outcomes will determine how widely the approach can be offered. For Grace Bell and her partner — who live in Kent — Hugo's arrival has completed a long journey that included being told at 16 that Bell would not be able to carry a child because she has MRKH syndrome, a condition in which a person is born without a viable womb and which affects one in every 5, 000 women in the UK.
Recent updates indicate this area of medicine remains under active research; details may evolve as the trial continues and as teams gather longer-term data on outcomes for mothers and children.