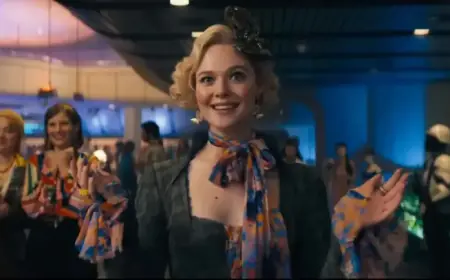Womb Transplant Baby Born: UK First as Hugo Arrives after Deceased Donor Uterus
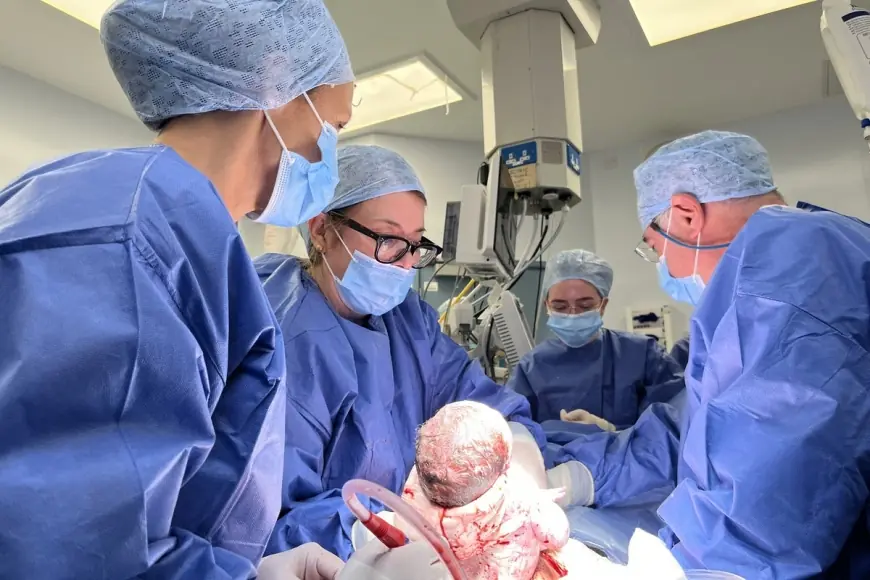
Grace Bell has become the first woman in the UK to give birth after receiving a womb transplanted from a deceased donor, a development that medical teams describe as ground‑breaking. The womb transplant baby born, Hugo, arrived in December at Queen Charlotte’s and Chelsea Hospital and the birth underscores both the technical challenges of deceased‑donor retrieval and the wider implications for family formation and organ donation policy.
Hugo born at Queen Charlotte’s and Chelsea Hospital
Hugo Powell was delivered at Queen Charlotte’s and Chelsea Hospital in west London in December, weighing 3. 09kg (6lb 13oz). Bell, now in her 30s, said seeing her son waking beside her felt like a dream and described the moment as “simply a miracle. ” The child is now 10 weeks old.
Grace Bell’s June 2024 transplant at The Churchill Hospital
Bell’s womb transplant took place in June 2024 at The Churchill Hospital in Oxford and lasted 10 hours. She began fertility treatment several months after the operation and underwent embryo transfer at The Lister Fertility Clinic in London, which led to the pregnancy carried in the transplanted uterus.
Prof Richard Smith, Womb Transplant UK, and the donor family
The couple, Grace and her partner Steve Powell from Kent, chose the middle name Richard for Hugo in recognition of Prof Richard Smith, clinical lead at the charity Womb Transplant UK and a consultant gynaecological surgeon at Imperial College Healthcare NHS Trust, who was present at the birth. Bell has publicly thanked the deceased donor and her family for what she called an “incredible gift. ” The donor’s parents said losing their daughter has shattered their world, but that through organ donation she has left a legacy that touches lives; five other organs from the same donor were transplanted into four people.
Isabel Quiroga and Oxford Transplant Centre on timing and risk
Isabel Quiroga, consultant surgeon and clinical lead for organ retrieval at the Oxford Transplant Centre within Oxford University Hospitals, emphasised the narrow window for using a uterus from a deceased donor, estimating the usable period at about 12 hours. She noted that internationally there have been more early failures after deceased‑donor uterine transplants than after living donations, making rapid coordination and specialist surgical teams essential to success.
Clinical pathway, monitoring and team effort
Clinicians described the case as the first UK birth from a deceased uterine donor, one of only a handful in Europe. The procedure sits inside a UK clinical research trial that plans for 10 transplants; three transplants have already been performed and this marks the first live birth from those efforts. More than 30 expert staff are involved in the care of each womb transplant patient, and teams provide additional appointments, extra scans and regular blood tests to monitor pregnancies after transplantation. Bryony Jones, a consultant obstetrician at Imperial College Healthcare NHS Trust who has delivered both babies born in the UK following womb transplants, said the work depends on voluntary contributions from clinicians alongside formally trained transplant and obstetric teams.
Because a transplanted womb requires immunosuppression, the medical plan is to remove the organ once the couple have finished having children to avoid lifelong immunosuppressant therapy.
Context: MRKH, earlier UK cases and international figures
Bell was born without a viable womb and does not have periods but retains normal ovarian function, a condition identified as Mayer‑Rokitansky‑Küster‑Hauser (MRKH) syndrome, which affects about 1 in 5, 000 women in the UK. As a teenager she was told she would be unable to carry a child, leaving her options as either surrogacy or a transplant. The UK’s first womb transplant in 2023 involved Grace Davidson receiving a living donation from her sister Amy. Internationally, roughly 25 to 30 babies have been born from deceased‑donor wombs; the majority of womb transplants overall use living donors while about a third use deceased donors. Because the uterus is not covered by typical organ‑donation consent mechanisms or by deemed consent, families are asked specifically to approve womb donation at the time of retrieval.
What makes this notable is the convergence of surgical timing, complex fertility care and organ‑donation logistics: the limited usable window for a deceased donor uterus, the 10‑hour transplant operation, and seamless follow‑up fertility treatment together produced a successful pregnancy and birth that clinicians call a potential model for others facing similar infertility.