Why it's a bit surprising that the U.S. is attending a key global flu meeting — Flu Shots influence and who feels it first
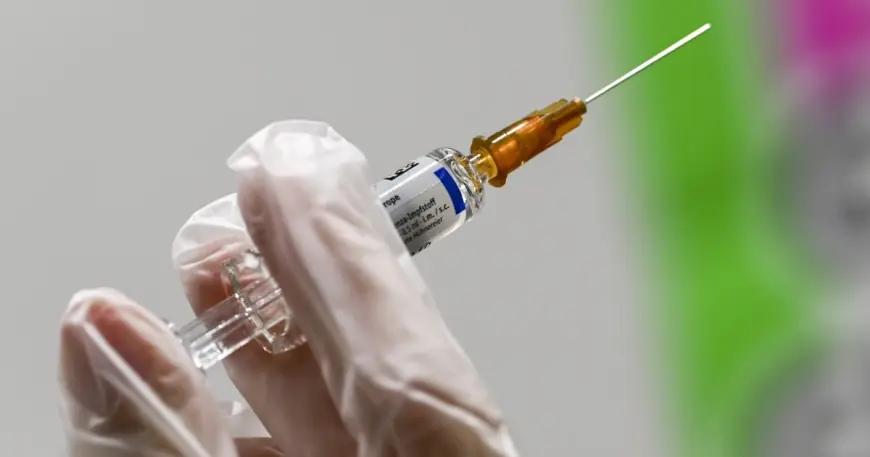
What matters now is practical: a thinner stream of virus samples and a more limited U. S. presence could change the clarity of the picture used to pick strains for flu shots aimed at fall 2026. Over the past week, about 50 flu scientists gathered in Istanbul to choose vaccine targets; the U. S. will take part with CDC staff joining remotely after an official withdrawal from the WHO in January. That mix — fewer samples plus virtual participation — shifts who feels the immediate effects.
Flu Shots: who experiences the shift and how surveillance gaps show up
Here’s the part that matters: the global system that informs vaccine strain selection depends on continuous data flows. The WHO’s surveillance system collects samples year-round from 130 countries and routes many of those to seven larger labs, among them the CDC. When the U. S. — historically a major funder — pulled out last year, shipments of samples slowed because of the loss of U. S. dollars. Fewer samples mean a dimmer view of how the virus is evolving, which can make it harder to pick the right strains for flu shots.
Who feels that first? Public health authorities that rely on timely, representative surveillance data; the labs that synthesize and interpret those samples; and populations targeted by vaccines chosen from a smaller evidence base. The meeting’s design work aims to create a shot for the next season, but the less robust the input data, the more constrained that design process becomes.
It’s easy to overlook, but the WHO pays for the shipments of samples — when those payments were disrupted, circulation of samples dipped. Officials have said shipments have since resumed, yet the interruption illustrates how funding shifts ripple through surveillance and vaccine planning.
What happened in Istanbul and how the U. S. is participating
For the past week, roughly 50 flu scientists have been meeting in a conference room at a Hilton hotel in Istanbul. Their goal is to select strains and design a vaccine intended to offer the best protection for the next flu season, starting in the fall of 2026. The World Health Organization convenes this meeting twice a year as part of its Global Influenza Surveillance and Response System.
In prior years, CDC scientists played a major role in these twice-yearly deliberations. After an official U. S. withdrawal from the WHO in January, the administration confirmed that CDC would send staff to take part, but the participation will be virtual rather than in person. The Department of Health and Human Services framed that participation as technical: contributing expertise, sharing surveillance data, and joining scientific discussions that inform vaccine strain recommendations, while noting the move does not change the withdrawal status.
- Meeting setting: ~50 scientists in Istanbul working on a vaccine for fall 2026.
- Surveillance scope: sample data collected year-round from 130 countries and analyzed at seven larger labs, including the CDC.
- Funding impact: a dip in sample shipments followed the loss of U. S. funding; shipments have been described as resumed.
Designing a vaccine is painstaking: one participant who previously led the CDC’s National Center for Emerging and Zoonotic Infectious Diseases described the work as "really tedious, " noting careful review of data is required to make the best choices for vaccine composition.
The real question now is whether virtual participation and a temporarily reduced flow of samples will alter the scientific balance at a moment when the meeting’s recommendations set the course for next season’s flu shots. An epidemiologist noted the practical reality that multi-country networks are central to protection efforts, even if political stances shift.
Micro timeline: over the past week scientists met in Istanbul; the meeting feeds recommendations used to design a vaccine for the fall 2026 season; surveillance is collected year-round from 130 countries. The overall schedule is part of a twice-yearly WHO cadence and is subject to change.
What’s easy to miss is how a short funding interruption can create longer-term visibility gaps: even a brief slowdown in sample circulation reduces the dataset available to labs making strain recommendations, and that reduced clarity can matter when building flu shots for an entire season.